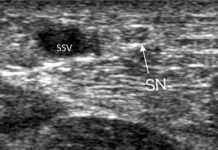
A recent study in the Journal of Vascular Surgery: Venous and Lymphatic Disorders highlights an important clinical reality:
In patients with post-thrombotic syndrome (PTS), the presence of the Great Saphenous Vein (GSV) may significantly influence ulcer healing and long-term outcomes.
Traditionally, a refluxing GSV is considered pathological and often treated accordingly. However, this assumption becomes questionable when venous hemodynamics are altered.
When deep venous outflow is compromised after thrombosis, the GSV may no longer function simply as a source of reflux. It may serve as a compensatory outflow pathway, helping maintain venous return.

The study by Bishara et al. compared PTS patients with active venous ulcers (CEAP C6) and found:
- Healing rate: 97% with preserved GSV vs 71% without
- Median healing time: 42.5 vs 161 days
- Recurrence/non-healing: 27% vs 85%
Notably, these differences persisted even when the GSV was refluxing—as long as it remained patent.
This suggests a key point: Functional contribution may be more important than structural perfection.
From a clinical perspective, this challenges a familiar approach.
The decision to treat the GSV should not rely solely on the presence of reflux.
A more relevant question is:
Does this vein still contribute to venous return?
If so, its removal may reduce the system’s ability to adapt—particularly in a limb already compromised by PTS.
PTS is a progressive condition. Future deterioration or recurrent thrombosis is always possible. In this context, preserving venous pathways is not only about current outcomes, but also about future reserve.
Once the GSV is removed, that reserve is lost.
Commentary
This study reinforces a broader shift in venous surgery:
From eliminating abnormal veins to understanding and preserving functional pathways
At the time of intervention, we are not only treating the present—we are shaping the patient’s long-term capacity to respond to disease.